What Is a Sleep Study and Why Is It Necessary?

Do you often wake up with a headache, startle awake in the middle of the night, or find yourself feeling exhausted by mid-day? There’s a good chance you could have sleep apnea, but the only way to know for sure is by receiving a diagnosis after a sleep study.
My dental practice in Cary, NC, regularly welcomes patients who suspect they may have a sleep disorder. My knowledge of the anatomy of the jaw and oral structures allows me to identify telltale signs, such as worn teeth and improper jaw positioning. If these signs are present, I can arrange for a sleep study with a local sleep doctor for an official diagnosis.
If you’re curious about what a sleep study is and why it’s necessary for diagnosing sleep apnea, you’re far from the first patient to ask. Here, I’ll break down how sleep studies work, signs you may need a sleep study, and the treatment options my Cary practice can help you with after you receive a diagnosis.
What Is a Sleep Study?
Simply put, a sleep study is an overnight medical examination during which a sleep doctor monitors various vital signs for disruptions or abnormalities while you are asleep. These signs include but are not limited to:
- Your heart rate
- Your breathing
- Your eye movement
- Your limb movement
- Your brain waves
- Your blood oxygen levels
Who Can Perform a Sleep Study?
This is an important point to address early on. North Carolina has laws regulating sleep apnea diagnosis. A diagnosis cannot be provided by dentists like myself, only by physicians. However, as a dentist who has extensively studied sleep–breathing disorders since 1992, I have helped a number of patients just like you with preliminary sleep apnea screenings.
I have also developed relationships with highly trusted sleep doctors throughout the Cary and Raleigh–Durham area, so I can easily connect you with a qualified professional for a sleep study if I see signs of the condition during your screening.
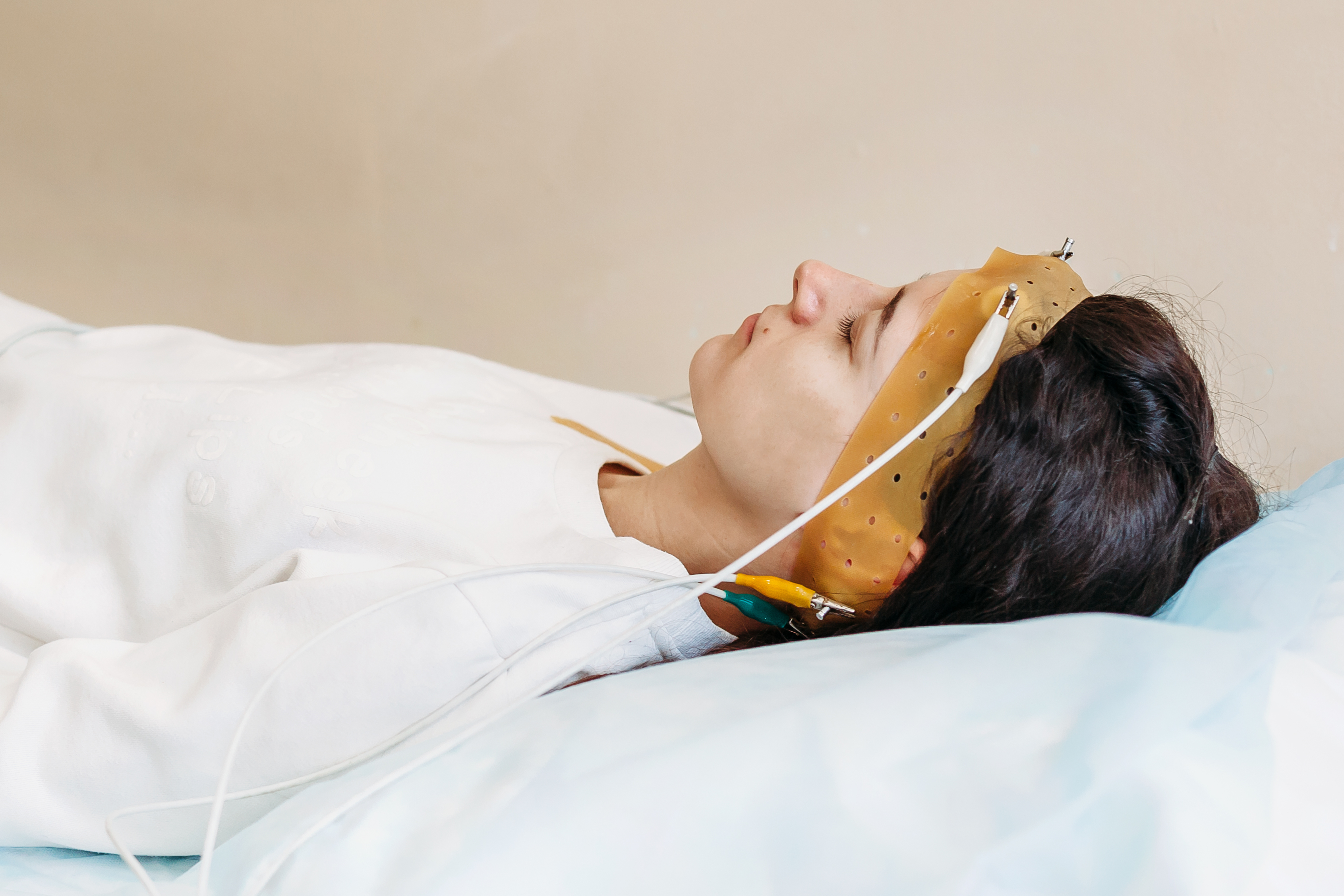
What Happens During a Sleep Study?
Sleep tests are totally non-invasive; there are no needles or injections involved, just monitoring equipment and gentle adhesives to hold some of the sensors in place.
Let's go step by step through the process.
1. Arrival at the Sleep Center or Hospital
Most sleep studies take place at a hospital or a sleep center. You will arrive at the facility in the evening and meet the technicians who will monitor your vitals overnight. They will explain the various tests to be run and the equipment used to run them, which typically includes:
- An electrocardiogram (ECG or EKG) to record cardiac activity
- An electrooculogram (EOG) to monitor eye activity
- An electroencephalogram (EEG) to measure brain activity
- A pulse oximeter to measure blood oxygen levels
2. Setting Up Equipment and Preparation
The technicians will bring you to a quiet, private room with a bed and simple amenities. They will set up the equipment and attach sensors to various parts of your body. After checking on your comfort and answering any questions you may have, they will leave you alone to relax and fall asleep at your own pace. The technicians will use audio and visual monitoring to watch over you from another room.
3. Monitoring Vital Signs and Eye Movement
Throughout the night, the sleep technicians will keep an eye on your vital signs and measure the number of waking events you experience. Though they may have to enter the room a few times to adjust the equipment, they will be quiet and interfere with your sleep as little as possible. It’s okay if you find it difficult to get a full night of sleep in a new environment. Even just a few hours of quality sleep will provide enough data to provide a diagnosis.
4. The Next Morning
The technicians will wake you early in the morning, typically after about six to eight hours of monitoring. You’ll be able to shower, enjoy a simple breakfast, and ask any final questions before leaving. Some patients choose to take the rest of the day off from work or school to readjust after a night in an unfamiliar environment, but you can absolutely carry out your day as normal afterward if you choose.
5. Diagnosis Based on Sleep Study Data
The technicians will take all the data collected throughout the night and send it to your sleep doctor, who will evaluate it to determine whether you have sleep apnea. This process usually takes about two weeks. If you do receive a diagnosis, you and I can discuss what the most effective treatment option may be at a follow-up appointment at my office.
Are Sleep Tests Uncomfortable?
No. Sleep tests are totally non-invasive; there are no needles or injections involved, just monitoring equipment and gentle adhesives to hold some of the sensors in place. You won’t have to worry about any discomfort except for adjusting to wearing the equipment and potentially being in a different environment for one night of sleep.
I say potentially because there is an alternative to a hospital- or facility-based study: the at-home sleep study. I work closely with sleep doctors who also offer the option of testing from the comfort of your own home and bed. This option is not best for all patients and all types of sleep apnea, so we can discuss which is right for you during your consultation.
Signs You May Need a Sleep Study for Sleep Apnea
Wondering how to know whether you need a sleep study in the first place? If you notice any of these telltale signs of sleep apnea, come visit me at my Cary office for a preliminary check.
- Waking with a start or a gasp during the night
- Waking up with a headache in the morning
- Waking up with a dry mouth or throat
- Loud, prolonged snoring
- Frequent daytime sleepiness
- Forgetfulness and mood swings
We’ll discuss your symptoms, and I’ll also examine your teeth and jaw for wear and misalignment, which can affect the flow of breath through your airways. It’s at this point that I can connect with a sleep doctor to arrange your sleep study.
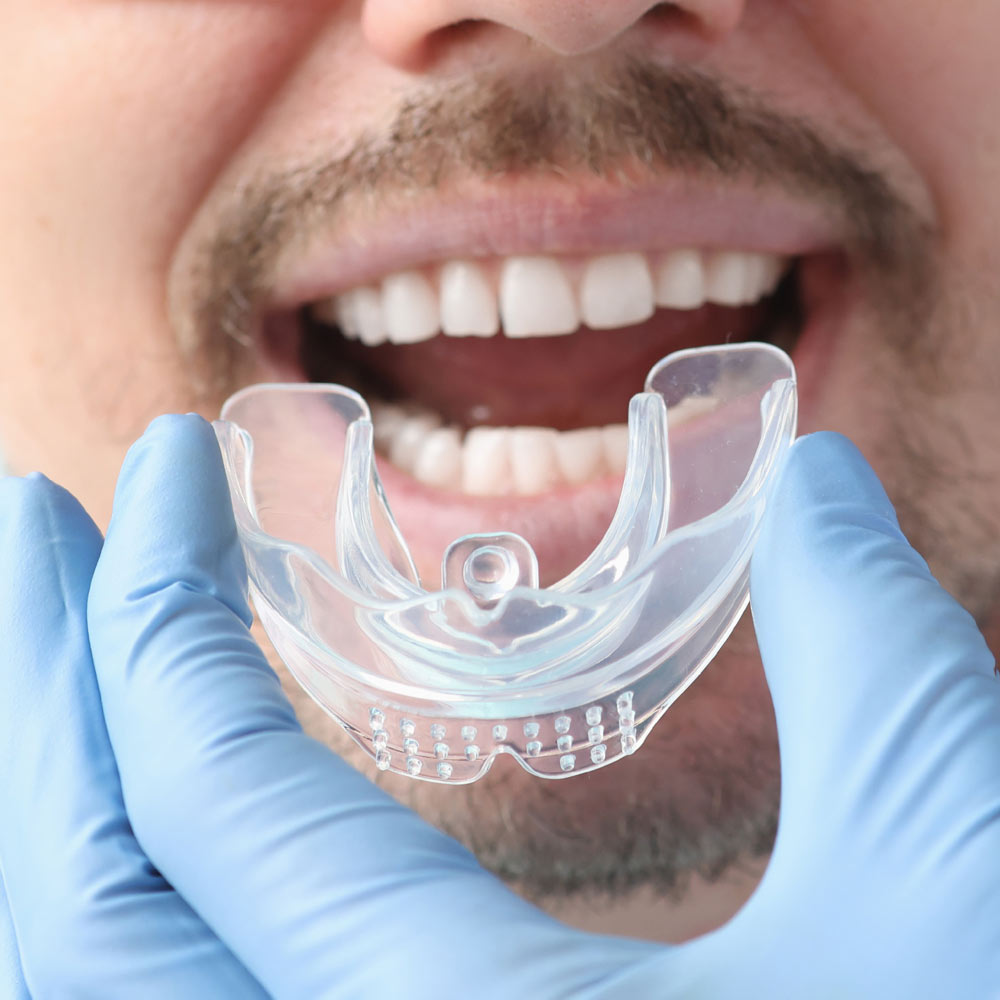
Sleep Apnea Treatment Options After Your Sleep Study
Though I cannot officially diagnose your sleep apnea, I can certainly help you treat it. Here are the three best options for obstructive sleep, by far the most common form of the condition:
- Lifestyle Changes: Many patients experience significant improvement in their sleep apnea symptoms after making a few small but key lifestyle changes. If you drink or smoke, cutting back can bring improvements to your sleep cycle, sleep quality, and ability to breathe during sleep. Increasing physical activity and losing excess weight can also be a big help.
- CPAP: A continuous positive airway pressure (CPAP) machine delivers oxygen to your airways through a mask or nosepiece worn during sleep. The gentle yet continuous pressure is effective at keeping the airways open, but it can take some time to adjust to the machine.
- Custom Oral Appliance: I can design and craft a personalized mouthguard-like appliance for you to wear while you sleep. This appliance will slightly move your jaw forward while worn, which repositions your airways for better airflow. Because it’s custom-designed for you, your mouthpiece will offer a comfortable fit. This is the most popular treatment option at my practice and my top recommendation for obstructive sleep apnea.
Suspect You Have Sleep Apnea? We Can Help. Get in Touch Today
Arranging for a sleep study on your own can be tricky, but you don’t have to. Helping patients with sleep and breathing disorders is one of my passions and specialities, and I’d love to help you as well. All you have to do is reach out to my dental practice in Cary, NC, for an initial sleep apnea consultation.
Allow me to coordinate accurate, efficient care for sleep apnea on your behalf. Send my team a message online or give our office a call today.

About Jeffrey S. Kearney, DDS
A dentist since 1992, Dr. Jeffrey Kearney has extensive training in TMJ and sleep-breathing disorders. He is a member of the Academy of General Dentistry and a fellow of the American Academy of Craniofacial Pain and the International Congress of Oral Implantologists.
Read Dr. Kearney's Full Bio | All Posts by Jeffrey Kearney